Diabetes complications
Understanding Hypoglycemia: A Comprehensive Guide
Hypoglycemia, also known as low blood sugar, is a common and potentially dangerous complication of diabetes. It occurs...
Understanding Eye Complications in Diabetes Patients
Diabetes is a chronic disease that affects millions of people worldwide, with numbers only continuing to rise. While most ...
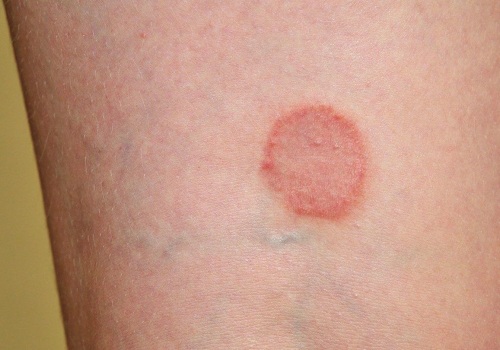
Understanding Skin Complications Associated with Diabetes
Welcome to our article on understanding skin complications associated with diabetes. As we all know, diabetes is a...
Understanding Hyperglycemia: What You Need to Know
Hyperglycemia is a common occurrence in individuals with diabetes, and it is important to understand what it is and how...
Understanding Kidney Disease: Types, Management, and Prevention
Diabetes is a chronic disease that affects millions of people worldwide. It is characterized by high levels of sugar in...
Understanding Ketoacidosis: A Comprehensive Guide for People with Diabetes
Diabetes is a chronic condition that affects millions of people worldwide. It occurs when the body is unable to produce...
Understanding Nerve Damage in Diabetes Patients
Diabetes is a chronic disease that affects millions of people worldwide. It is characterized by high levels of sugar in...
Understanding Cardiovascular Disease
Welcome to our comprehensive guide on understanding cardiovascular disease, one of the most common and serious health...